The United Nations predicted 7 million additional unintended pregnancies would occur if the coronavirus lockdown lasted 6 months. It is already more than a half year since the pandemic started, but we won’t know the effects on reproductive health services for months to come.
Part of the problem accessing care in developing countries is what are called “stock-outs”. Where the supply chain is long, supplies often run out. An example of the impact of this problem is that a woman may spend a day and money for the bus to go to the family planning clinic for her 3-monthly shot of DepoProvera, and find out that the clinic has run out of the medicine.
One solution for this has been explored. Another form of Depo has been developed which also lasts 3 months, is highly effective, but is given under the skin rather than into the muscle. An “appropriate technology” way to package this subcutaneous shot. Sayana® Press is a single-use syringe that contains the medication in a small plastic capsule attached to the short needle. All the woman needs to do after placing the needle is to squeeze the capsule.
Women in Malawi are first taught how to give themselves the injection, then supervised as they actually do it. Then they are given 3 syringes to take home. It was found that self-injection works well and was more popular with women than having to make 4 trips each year. As a consequence, the continuation rate was higher among women who only visited the clinic annually.
With the pandemic there are many other reasons than stock-outs that can make it impossible for people to get the most effective, modern family planning. The clinic may be closed, the bus driver sick or the family has run out of money. Many providers, myself included, have disparaged traditional methods of contraception because of their lack of effectiveness. However, during a time of emergency such as the pandemic, any family planning method is better than none for a couple who wants to postpone pregnancy. Knowledge of traditional contraception helps to prepare for disruptive events.
Many societies have ways of controlling fertility. These include breastfeeding, prolonged abstinence from intercourse after childbirth, abstinence during the fertile time in a woman’s cycle (often called “natural family planning” or “the rhythm method”), and withdrawal.
It has been known for centuries that nursing a baby makes the mother relatively infertile; the Lactational Amenorrhea Method (LAM) formalizes this knowledge. LAM is 96% effective if: the baby is less than 6 months old, is nursing with little supplementation and the woman hasn’t started to menstruate yet. The reduction of fertility is less, but still significant, if only 1 or 2 of the criteria are met.
The effectiveness of periodic abstinence is debated. What is not debated, however, is that instruction in the method is helpful, and that a cooperating partner is essential. Some studies report almost 100% effectiveness, while others cite much lower figures. There are many ways of tracking when a woman is fertile, and each has its own success rate–but most are in the range of 80%. This means that about 20 out of 100 women will get pregnant when using periodic abstinence.
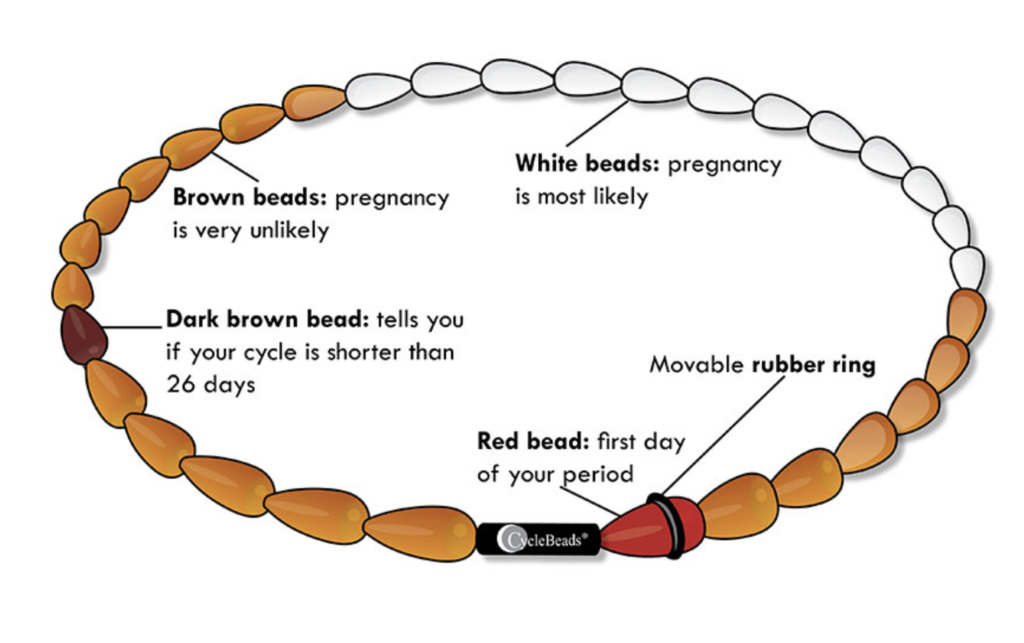
There are two ways of increasing effectiveness of periodic abstinence. Users of the Standard Days Method® (formalized by using CycleBeads®) report an effectiveness approaching that of modern contraception, but it is limited to women who have 26 to 32-day cycles. The other is with a smartphone app. CycleBeads has one, and there are many others. One, Natural Cycles, is FDA approved and claims to be over 90% effective in preventing pregnancy.
Withdrawal (pulling out”) has the distinction of being so old that it is mentioned in Genesis. It is a family planning method that needs no medication or supplies, just perception and willpower on the man’s part. He needs to perceive when ejaculation is imminent and withdraw his penis before it occurs. Overall, withdrawal is about 80% effective. However, for a man who uses this method perfectly, his partner only has a 4% risk of conceiving each year. As I found out in Puerto Rico where many of my patients used withdrawal, in certain populations it may be very effective.
An article in The Economist “The pandemic may be leading to fewer babies in rich countries brings no surprise,” the birth rate seems to be down in rich countries, but people in poor countries are probably having more babies. Covid is increasing problems for the poor.
© Richard Grossman MD, 2020